To test the effects of different vaccination advocacy message strategies on attitudes toward HPV vaccination, we randomly assigned study participants (N = 963) to one of four different message-strategy groups:
(1) The Narrative Strategy–A short story about a parent, Mark, who takes his 11-year-old daughter Emma to the doctor. During the visit, the doctor recommends that Emma receive the HPV vaccination. Mark is at first hesitant, but after considering the facts the doctor tells him, he decides to get Emma vaccinated. Afterward, they go for ice cream.
(2) The Informative Strategy–A fact-and-figure-filled overview of the case for HPV vaccination based on reports from the CDC, including the range of cancers the vaccination would prevent, the number of lives it would save, and its excellent safety record.
(3) The Expert Strategy–An appeal from a doctor with an impressive-sounding title asking for support in gaining acceptance for HPV vaccination, citing similar facts and figures from CDC reports. Accompanying the appeal was a photo of a distinguished-looking male doctor.
(4) The Non-Expert Strategy–An appeal from a school PTA member asking for support in gaining acceptance for HPV vaccination, citing the exact same facts, figures and rationale as the appeal from the expert doctor. Accompanying the message was a photo of a young mother with a small daughter on her lap.
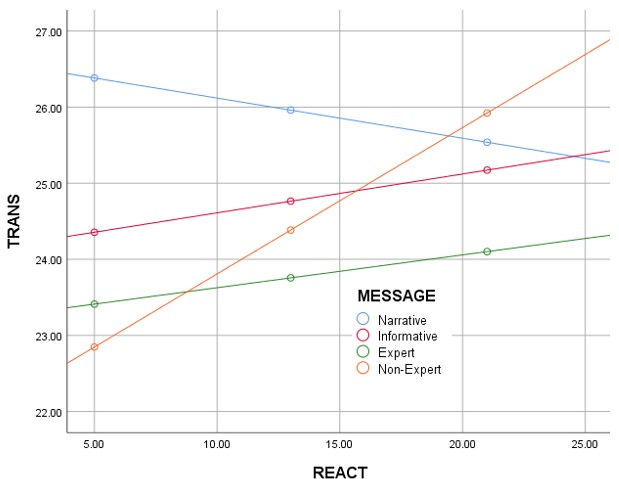
As illustrated in the graph above (Figure 1), when the vaccination advocacy messages focused on factual reasons for supporting HPV vaccination (as in the Informative, Expert spokesperson, and Non-Expert spokesperson message strategies), reactance (i.e., resistance) increased as transportation (i.e., emotional engagement with the message) increased. But when the message was delivered as a narrative story about one person’s HPV vaccination decision, reactance declined as transportation increased.
Resistance is persistent and problematic
HPV vaccinations are safe, readily available, and if universally administered would prevent countless cancers and save 4,000 or more lives in the U.S. every year. But at least 25% of the parents who receive vaccination recommendations from their doctors decline to have their children vaccinated.
Source: CDC (2019) Vaccine for human papillomavirus.
As the graph above (Figure 1) suggests, receiving vaccination advocacy recommendations from an informative source or an expert figure like a doctor produced significant amounts of resistance, with greater involvement in the message producing greater levels of resistance. Receiving those recommendations from a non-expert figure amplified this effect. But telling a story about a parent overcoming doubts to support HPV vaccination seemed to reverse this effect, with greater involvement in the story producing reduced amounts of reactance.
Analyses
The message strategies were modestly effective in producing positive attitude change: Post-Test Attitude – Pre-Test Attitude Mean Difference = 1.41 (SD = 3.81), t (935) = 11.34, p < .001. While there was no significant difference in attitude change between the messages, F (3, 932) = 0.79, p = .787, examination of the underlying factors contributing to attitude change revealed significant mediating effects of transportation and moderating effects of reactance.
While the direct effect of the different message strategies on attitude change was negligible, F (4, 931) = 2.08, p = .081, the indirect effect including the potentially causal mediating effect of transportation was quite significant, with greater levels of transportation producing greater change in attitude, t (933) = 2.75, p = .006. Greater levels of reactance, on the other hand, produced less and in fact negative change, t (933) = -4.92, p < .001.
Transportation vs. Reactance
With each of the typical persuasive message strategies that used facts and figures to achieve compliance with vaccination recommendations, as transportation (i.e., emotional engagement) increases, so does reactance (i.e., resistance), illustrated by the parallel lines that rise going from left to right in Figure 1. This increase in reactance limits the effectiveness of those messages to influence positive changes in attitude toward vaccination.
With the narrative strategy, on the other hand, increased emotional engagement with the story was associated with reduced reactance. This suggests storytelling may be an effective means for overcoming or avoiding resistance to vaccination when more directive strategies fail.
HPV Vaccination Background
Widely known to be the primary cause of cervical cancer, which kills more than 4,000 women in the United States each year (U.S. Cancer Statistics, 2019), HPV infection also causes cancer of the anus, penis and throat in men, and genital warts in both sexes (CDC, 2019). The infection is so widespread as to be considered of epidemic proportion. In the U.S., 80 million people (about one in four) are currently infected with HPV, 14 million more become infected each year, and nearly 35,000 people each year are affected by a cancer caused by HPV (CDC, 2019).
A widely available, easily affordable vaccine that would prevent 92% of HPV infections has been shown to be safe and effective (CDC, 2019), and the rational, socially responsible, utilitarian case for universal vaccination against HPV seems highly persuasive. However, acceptance and utilization of the vaccine have been far from universal. Barely half of 13-to-17-year-old adolescents in the U.S. are up-to-date on their vaccinations against HPV (Walker et al., 2019), and reports suggest that the percentage of parents actively choosing to resist having their children vaccinated against HPV is increasing (Darden et al., 2013.)
Explanations for the continued resistance and strategies for overcoming it are needed. The effects of reactance may be part of an explanation, and storytelling strategies may be part of the solution.
References
CDC (2019, August 2). Vaccine (shot) for human papillomavirus. Retrieved on March 17, 2021 from: https://www.cdc.gov/vaccines/parents/diseases/hpv.html
Darden, P.M., Thompson, D.M., Roberts, J.R., Hale, J.J., Pope, C., Naifeh, M., & and Jacobson, R.M. (2013). Reasons for not vaccinating adolescents: National Immunization Survey of Teens: 2008 – 2010, Pediatrics, 131, 645-651. Available online at http://pediatrics.aappublications.org/content/early/2013/03/12/peds.2012-2384
U.S. Cancer Statistics (2019, June). Leading cancer cases and deaths, female, 2016. U.S. Cancer Statistics Data Visualizations Tool, based on November 2018 submission data (1999-2016). U.S. Department of Health and Human Services, Centers for Disease Control and Prevention and National Cancer Institute. Retrieved from https://gis.cdc.gov/Cancer/USCS/DataViz.html
Walker, T.Y., Elam-Evans, L.D., Yankey, D., Markowitz, L.E., Williams, C.L., Fredua, B., Singleton, J.A., & Stokley, D. (2019, August 23). National, regional, state, and selected local area vaccination coverage among adolescents aged 13-17 years—United States, 2018. Morbidity and Mortality Weekly Report (MMWR), Centers for Disease Control and Prevention (CDC). Retrieved from https://www.cdc.gov/mmwr/volumes/68/wr/mm6833a2.htm