Home » Health Communication
Category Archives: Health Communication
Tell me a story about getting vaccinated
To test the effects of different vaccination advocacy message strategies on attitudes toward HPV vaccination, we randomly assigned study participants (N = 963) to one of four different message-strategy groups:
(1) The Narrative Strategy–A short story about a parent, Mark, who takes his 11-year-old daughter Emma to the doctor. During the visit, the doctor recommends that Emma receive the HPV vaccination. Mark is at first hesitant, but after considering the facts the doctor tells him, he decides to get Emma vaccinated. Afterward, they go for ice cream.
(2) The Informative Strategy–A fact-and-figure-filled overview of the case for HPV vaccination based on reports from the CDC, including the range of cancers the vaccination would prevent, the number of lives it would save, and its excellent safety record.
(3) The Expert Strategy–An appeal from a doctor with an impressive-sounding title asking for support in gaining acceptance for HPV vaccination, citing similar facts and figures from CDC reports. Accompanying the appeal was a photo of a distinguished-looking male doctor.
(4) The Non-Expert Strategy–An appeal from a school PTA member asking for support in gaining acceptance for HPV vaccination, citing the exact same facts, figures and rationale as the appeal from the expert doctor. Accompanying the message was a photo of a young mother with a small daughter on her lap.
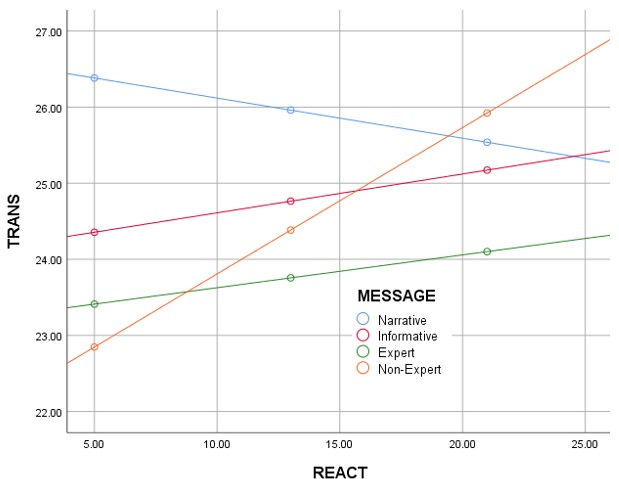
As illustrated in the graph above (Figure 1), when the vaccination advocacy messages focused on factual reasons for supporting HPV vaccination (as in the Informative, Expert spokesperson, and Non-Expert spokesperson message strategies), reactance (i.e., resistance) increased as transportation (i.e., emotional engagement with the message) increased. But when the message was delivered as a narrative story about one person’s HPV vaccination decision, reactance declined as transportation increased.
Resistance is persistent and problematic
HPV vaccinations are safe, readily available, and if universally administered would prevent countless cancers and save 4,000 or more lives in the U.S. every year. But at least 25% of the parents who receive vaccination recommendations from their doctors decline to have their children vaccinated.
Source: CDC (2019) Vaccine for human papillomavirus.
As the graph above (Figure 1) suggests, receiving vaccination advocacy recommendations from an informative source or an expert figure like a doctor produced significant amounts of resistance, with greater involvement in the message producing greater levels of resistance. Receiving those recommendations from a non-expert figure amplified this effect. But telling a story about a parent overcoming doubts to support HPV vaccination seemed to reverse this effect, with greater involvement in the story producing reduced amounts of reactance.
Analyses
The message strategies were modestly effective in producing positive attitude change: Post-Test Attitude – Pre-Test Attitude Mean Difference = 1.41 (SD = 3.81), t (935) = 11.34, p < .001. While there was no significant difference in attitude change between the messages, F (3, 932) = 0.79, p = .787, examination of the underlying factors contributing to attitude change revealed significant mediating effects of transportation and moderating effects of reactance.
While the direct effect of the different message strategies on attitude change was negligible, F (4, 931) = 2.08, p = .081, the indirect effect including the potentially causal mediating effect of transportation was quite significant, with greater levels of transportation producing greater change in attitude, t (933) = 2.75, p = .006. Greater levels of reactance, on the other hand, produced less and in fact negative change, t (933) = -4.92, p < .001.
Transportation vs. Reactance
With each of the typical persuasive message strategies that used facts and figures to achieve compliance with vaccination recommendations, as transportation (i.e., emotional engagement) increases, so does reactance (i.e., resistance), illustrated by the parallel lines that rise going from left to right in Figure 1. This increase in reactance limits the effectiveness of those messages to influence positive changes in attitude toward vaccination.
With the narrative strategy, on the other hand, increased emotional engagement with the story was associated with reduced reactance. This suggests storytelling may be an effective means for overcoming or avoiding resistance to vaccination when more directive strategies fail.
HPV Vaccination Background
Widely known to be the primary cause of cervical cancer, which kills more than 4,000 women in the United States each year (U.S. Cancer Statistics, 2019), HPV infection also causes cancer of the anus, penis and throat in men, and genital warts in both sexes (CDC, 2019). The infection is so widespread as to be considered of epidemic proportion. In the U.S., 80 million people (about one in four) are currently infected with HPV, 14 million more become infected each year, and nearly 35,000 people each year are affected by a cancer caused by HPV (CDC, 2019).
A widely available, easily affordable vaccine that would prevent 92% of HPV infections has been shown to be safe and effective (CDC, 2019), and the rational, socially responsible, utilitarian case for universal vaccination against HPV seems highly persuasive. However, acceptance and utilization of the vaccine have been far from universal. Barely half of 13-to-17-year-old adolescents in the U.S. are up-to-date on their vaccinations against HPV (Walker et al., 2019), and reports suggest that the percentage of parents actively choosing to resist having their children vaccinated against HPV is increasing (Darden et al., 2013.)
Explanations for the continued resistance and strategies for overcoming it are needed. The effects of reactance may be part of an explanation, and storytelling strategies may be part of the solution.
References
CDC (2019, August 2). Vaccine (shot) for human papillomavirus. Retrieved on March 17, 2021 from: https://www.cdc.gov/vaccines/parents/diseases/hpv.html
Darden, P.M., Thompson, D.M., Roberts, J.R., Hale, J.J., Pope, C., Naifeh, M., & and Jacobson, R.M. (2013). Reasons for not vaccinating adolescents: National Immunization Survey of Teens: 2008 – 2010, Pediatrics, 131, 645-651. Available online at http://pediatrics.aappublications.org/content/early/2013/03/12/peds.2012-2384
U.S. Cancer Statistics (2019, June). Leading cancer cases and deaths, female, 2016. U.S. Cancer Statistics Data Visualizations Tool, based on November 2018 submission data (1999-2016). U.S. Department of Health and Human Services, Centers for Disease Control and Prevention and National Cancer Institute. Retrieved from https://gis.cdc.gov/Cancer/USCS/DataViz.html
Walker, T.Y., Elam-Evans, L.D., Yankey, D., Markowitz, L.E., Williams, C.L., Fredua, B., Singleton, J.A., & Stokley, D. (2019, August 23). National, regional, state, and selected local area vaccination coverage among adolescents aged 13-17 years—United States, 2018. Morbidity and Mortality Weekly Report (MMWR), Centers for Disease Control and Prevention (CDC). Retrieved from https://www.cdc.gov/mmwr/volumes/68/wr/mm6833a2.htm
The Last Word on Improving Patient Satisfaction
You’ve improved your patient-care processes and outcomes but you’re still not happy with your patient satisfaction scores. And now, with CMS reimbursements increasingly tied to those scores, the pressure is rising to raise them.
Fortunately, the fields of psychology and behavioral economics may offer some easy-to-implement solutions to improve patient satisfaction scores both coming and going.
Start at the beginning
People’s memories are selective. They remember the beginnings and endings of things far more vividly and intensely than the middles.
The beginnings are particularly important, because they set up the patient’s expectations for everything that is to follow. It’s called “affect priming.”
If the beginning is stressful and unpleasant, the rest of the stay will have much repair work to do. Therefore, it is crucial to address patient satisfaction from the very beginning—the patient’s arrival at the hospital.
Address the parking situation: Worrying about finding a place to park is an issue that affects patients as well as their families. A free valet parking service can remove this worry and help create a caring first impression.
Careful maintenance of parking lots—to make them easily accessible, clean and safe— and liberal parking validation policies will also address this important opportunity to make a good first impression.
Greet everyone with a “Hello, can I help you?” Even people who spend a lot of time visiting hospitals can have a hard time finding their way around. Making every visitor feel welcomed and taken care of must become everyone’s priority.
Specially trained volunteers and/or dedicated staff “Welcome Ambassadors” can make a real difference in visitors’ experience.
Add some branded swag to the intake and admission process: In addition to making people feel welcome, giving them some branded items at intake can help them feel a stronger and more positive connection to you.
The act of accepting the gift of a branded pen (and/or other items such as tote-bags, socks, tee-shirts, baseball hats etc.) creates a sense of endorsement and mutual regard on the part of a patient. (It also helps if the intake and admission process is streamlined and friendly, of course!)
Your Last Chance
Research by Daniel Kahneman and Donald Redelmeier1 has shown the power of happier endings. They found that adding a period of greater comfort to the end of a painful experience influenced subjects to remember their pain levels as less intense.
Even when they made the overall unpleasant experience longer, ending it more pleasantly made the whole experience seem more pleasant.
The takeaway from this research is simple: Making the last few hours of a hospital stay more pleasant can change a patient’s lasting impression of the entire stay.
Here are a few last-day strategies that can pay big patient-satisfaction dividends:
Special last day meals: Food is always one of the most memorable (and not always pleasant) things about a hospital stay. Special meal treats on the last day before discharge, like an extra-specially made desert, can help make patients feel as though they have been treated with special care.
Special last day farewells: It is easy for a patient to feel anonymous, especially in a large institution like a hospital. Post the discharge schedule at all unit stations, and make it a priority for all members of every shift – and every discipline, including support and non-clinical personnel – to review the list and stop in to offer some “goodbye” best wishes.
The 30 seconds it will take will yield long-lasting and highly positive memories for the patient—and for your staff members as well.
Special last day treats and gifts: The same discharge schedule can be used as a distribution schedule for more branded swag items like those mentioned above in association with intake.
Tote bags are especially handy at discharge, especially if they are needed to carry some parting gifts—all carrying your hospital’s logo imprint, of course. Specially branded cookies and cupcakes (decorated with your logo as icing) can also help patients leave with good memories of their stay.
Health care includes showing you care
We’ve all seen studies that show that patients who have good communications with their care-givers rate the quality of care they receive higher. That’s another area worth focusing on for raising patient satisfaction scores (and certainly worth a few future posts).
Good communication makes for good relationships, and both circle back to the “affect priming” mentioned at the beginning of this post. If you show people you care about them on Day One, they will feel more cared about through their entire stay (and afterward, when they answer those HCAHPS survey questions).
You show you care by being interested—genuinely interested—in how they feel and what they have to say. Which means that it’s not enough to start off that first contact with, “Hello, can I help you?”
You also need to listen to what comes next.
References1
Kahneman, Daniel; Frederickson, Barbara L.; Schreiber, Charles A. & Redelmeier, Donald A. (1993) When more pain is preferred to less: Adding a better end. Psychological Science, 4(6), 401-405.
Redelmeier, Donald A. & Kahneman, Daniel (1996) Patients’ memories of painful medical treatments: real-time and retrospective evaluations of two minimally invasive procedures. Pain, 66(1), 3-8.
Reducing Risky Behavior
Risk Communication Can Be Risky
Environmental Safety and Public Health Policy-Makers Often Make Matters Worse
Communication of science-based information to the general public…particularly health-related information…is a well-studied field.
This may be because it is so often done so poorly.
Many public behavior interventions, especially those based on intuition, “common sense,” political persuasion or religious belief, tend to focus on presenting a rational, logical argument for complying with a specific behavioral request.
Researcher Timothy D. Wilson cites “D.A.R.E.” and “Scared Straight” interventions…famous and widely adopted programs intended to reduce crime and drug use among young people…as examples of programs that “make perfect sense, but… are perfectly wrong, doing more harm than good. It is no exaggeration to say that commonsense interventions [such as these] have prolonged stress, raised the crime rate, increased drug use, made people unhappy, and even hastened their deaths.” (Source: Wilson, 2011, Redirect: The surprising new science of psychological change. New York: Little, Brown & Co.)
Unfortunately, this “boomerang effect” is too common in public policy communications. Public policy communicators would do well to read the government’s own manual on risk communication, which ought to be stapled to every keyboard in every PR department in every science, health and environmental organization in the English-speaking world.
Risk Is Attractive
Nike’s 5-minute animated World Cup commercial urges its audience to “Risk Everything,” basically because the safe route is boring. And clearly, there are a lot of risk-seekers out there.
While the animation and execution are exquisite, the storyline is predictable to the nth degree—but who cares? As an exercise in appealing to its targeted demographic: GOOOAAAAAALLLLLLLL!
The product shots are also very appealing. These are not the soccer cleats I wore in high school, and the shirts and shorts look as though world-cup-worthy pectorals, abs and glutes are included at no extra charge.
All this being said, the spot ought to be worrisome to conservatives, control freaks (including many sports coaches) and public health advocates. The reason it should be worrisome is not because of the spot’s likely influence on an easily-manipulated demographic—actually, soccer players are a rather stubborn lot. This spot is not going to change them in any way except maybe to increase their motivation to buy another pair of cleats.
No, the scarier scenario is that the spot is an accurate reflection of the risk-seeking ethos of an entire generation. In the spot’s storyline, risking everything is the only way to beat the practiced but predictable perfection of the clones (who could also be the minions of the Matrix, or the Man, or your parents).
But in real life, the associated behaviors are:
- Going for the low-percentage spectacular dunk rather than the safe but boring lay-up
- Riding the motorcycle without the helmet
- Not buckling those seat belts
- Not vaccinating your kids
- Not stopping to unroll that Trojan
- Not settling for the status quo
Small wonder so many campaigns aiming to reduce risky behaviors actually serve to increase them. Maybe the control freaks and health communicators would do better if they positioned those undesired behaviors as something other than risky.
How about stupid? Or shameful? Or embarrassing?
As Nike is trying to tell them, risky is just too attractive.
The Politics of HPV Vaccination Advocacy
Who would YOU listen to?
A study of the influence of spokesperson expertise

My paper, “The politics of HPV vaccination advocacy: Effects of source expertise on the effectiveness of a pro-vaccine message,” was recently accepted for publication in the 71st Annual New York State Communication Association Conference Proceedings. The conference was held in Ellenville, NY, on October 18-20, 2013.
The paper received the conference’s award for Top Graduate Student Paper.
HPV (human papillomavirus) is a worldwide scourge that causes cervical cancer and thousands of deaths each year. Who do YOU think would be more influential in persuading people to support vaccination against HPV?
Most people would guess the authoritative-looking woman doctor on the left. After all, how much influence could a non-expert like the Middle School student on the right be expected to wield?
That was the focus of my study of spokesperson expertise.
Universal HPV vaccination would save more than 3,000 lives annually in the United States, and more than 350,000 worldwide. It makes sense. Its benefits seem almost inarguable. But there is a huge amount of opposition, largely distributed along political and ideological lines.
The intersection of health, science and politics
Mistrust and disbelief in evidence-based science and the recommendations of scientists are widespread and distributed along partisan lines. It is hard to prove any immediate life-and-death consequences to rejection of evolution or denial of the possibility of human agency in climate change. But with HPV and cervical cancer, the consequences are clear, present and immediate. We can document that partisan opposition to HPV vaccination is killing people right now.
The results of my study suggest that people who are inclined to oppose HPV vaccination are more likely to listen to and be influenced by pro-vaccination messages from an obviously non-expert spokesperson (in this study, an innocent-looking middle school student) than from an expert (in this study, an authoritative-looking woman doctor).
Three test groups: Expert, Non-Expert & Control
In my study, 474 adults were randomly divided into three groups. One group was instructed to read some basic, neutral information about the HPV virus and a pro-vaccination advocacy message attributed to the woman doctor.
A second group was instructed to read the same basic information about the HPV virus and the same pro-vaccination advocacy message, but for this group the message was attributed to the middle school student.
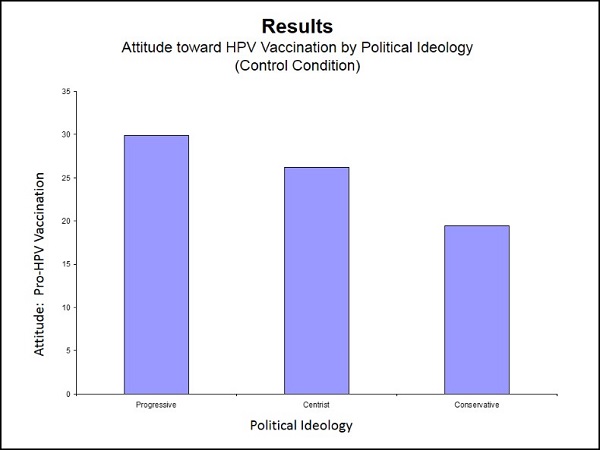
The third group (the control group) read the same basic information about the HPV virus, but received no advocacy message. Members of all three groups were also instructed to rate themselves politically as either Progressive, Centrist or Conservative.
After completing their reading assignments, the subjects were surveyed about their attitudes toward HPV vaccination.
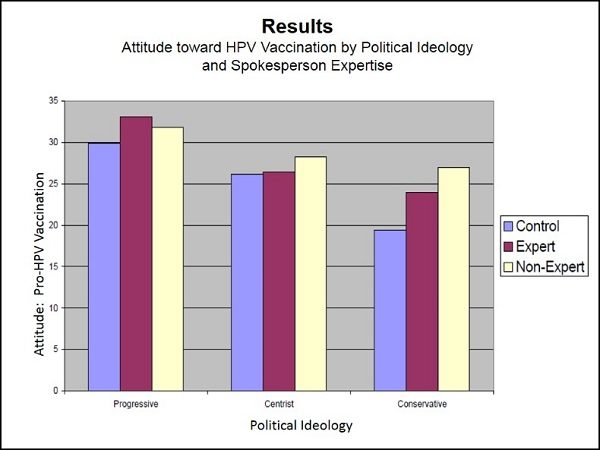
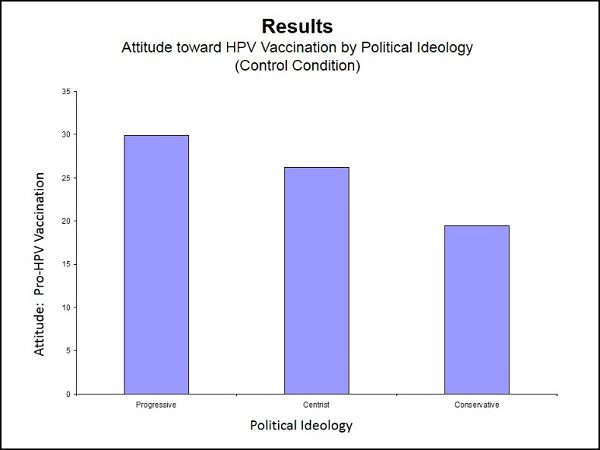
The attitude-scores of the control group (the ones who read only basic information but received no advocacy message) showed how attitudes toward HPV vaccination are skewed along partisan political lines. The more conservative the individual, the more opposed to HPV vaccination that person was likely to be.
Displaying the results for all three groups side-by-side (see chart below), it is clear that Centrists and Conservatives—those more likely to be opposed to vaccination—are more positively influenced by the Non-Expert spokesperson than the Expert.
For both Centrists and Conservatives, attitudes among those who read the advocacy message from the Non-Expert were significantly more positive than among those who received no advocacy message. There was no such significant difference in attitudes of those who read the advocacy message attributed to the Expert.
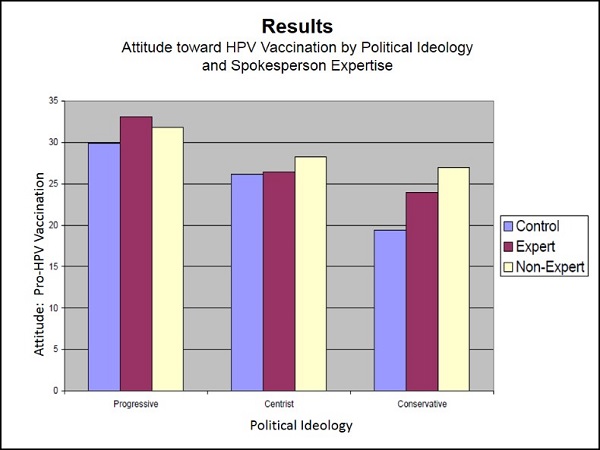
With Centrists, in fact, attitudes toward vaccination among those who received the advocacy message delivered by the Expert were virtually identical to those who received no advocacy message at all.
Among Progressives — who tend to favor HPV vaccination to begin with — attitudes toward HPV vaccination were more more positively influenced by the Expert than the Non-Expert.
Since virtually all pro-vaccination campaigns are spearheaded by people who favor vaccination, it seems likely that the tendency to rely on expert authorities as public advocates for vaccination may be the result of unexamined and untested assumptions that what influences Progressives will influence everyone. The power of spokesperson expertise may be overblown.
Overall, these results suggest that HPV vaccination advocates would be more successful if they would enlist more non-expert spokespeople in their public information efforts. The results also suggest that information about scientific and politically charged subjects might receive greater attention from doubters if the information is delivered by spokespeople who are not immediately identifiable as expert advocates for the other side.
Someone seeing the serious-looking doctor knows another authoritative persuasive argument is coming and tunes out before any persuasion can happen. With the non-threatening middle school student, there is more chance that the persuasive message will be heard.
Some persuasion is more effective than none!
A follow-up study suggested some interesting reasons for these results!
Reverse Psychology?
Yes, apparently you can actually get people to do something (or maybe NOT do something) by encouraging them to do the opposite.
There is a growing body of research that shows people can be discouraged from doing things they find pleasurable by paying them to do those things.
Theorists believe it demonstrates one of the major differences between intrinsic and extrinsic motivation.
When people do things because those actions give them pleasure or fulfillment, their motivations are intrinsic. Performing the actions becomes intertwined with their sense of identity: they do those things because of who they are.
When people do things because an outside force is compelling them to take those actions – by paying them, or forcing them or shaming them into it – their motivations are extrinsic. There is not the same kind of connection with the sense of identity.
With extrinsic motivation, there is often an undercurrent of resentment – psychological reactance – and a lost sense of freedom that can sap the pleasure out of an action that may have once been performed for fun. Extrinsic motivation tends to dampen and can even extinguish intrinsic motivation.
Putting this strategy into practice may be difficult, however. The chances of convincing any organization that must answer to public opinion to actually use this human tendency in an intentional way is pretty slim.
For instance, I don’t think we can convince the government that a good way to combat obesity would be to pay fat people to eat more.
But what about gun control?
Given the climate in the Republican-held House of Representatives, we are far more likely to pass a bill offering people financial incentives to own as many guns as possible than to pass a bill restricting gun rights in any way.
If we could get the government (i.e., the hated government, from which no good can ever come) to pay people to own guns, maybe this would work better to discourage gun ownership than trying to legislatively take away people’s right to bear arms.
By the way, on the subject of gun control, people on both sides of the debate could gain additional perspective on the matter by reading the classic science fiction novella, “The Weapon Shops of Isher,” by A.E. van Vogt.